
 IJCP Editorial Team
IJCP Editorial Team
Multiple developmental urogenital anomalies - A therapeutic challenge
Abstract
In cases of atretic lower vagina drainage of hematocolpos per se is inadequate as recurrent hematocolpos from restenosis is common. Surgical reconstruction in these cases should be directed to relieve obstruction and ensure continued vaginal patency. A 14 years old girl reported for primary amenorrhea and recurrence of cyclical lower abdominal pain due to restenosis following a primary intervention for hematocolpos. Evaluation identified an atretic lower vagina and multiple associated urinary tract anomalies like unascended right kidney, malrotated left duplex collection system, ureteric diverticula and bladder diverticlum with left ureter opening into it. Though associated grade IV vesicoureteral reflux (VUR) posed a management dilemma, drainage of hematocolpos and restoration of vaginal continuity by pull through of the proximal vagina and approximating its edges to fourchette relieved the patient of pain, restored menstruation, resolved the VUR and obviated the need for extensive urinary reconstructive procedures.
Introduction:
Occlusive vaginal anomaly is identified after puberty, with onset of menstruation when accumulation of menstrual blood causes pain.
Surgical management of combined multiple developmental anomalies may appear to be complex with prospect of multiple surgical corrections.
Case Report:
This manuscript was prepared after obtaining written informed consent from father of the patient. A 14 year old girl presented with primary amenorrhea and lower abdominal pain with cyclical increase in severity for three months. Patient did not have any voiding difficulty.
Occurrence of acute abdominal pain at her 14th year (1.12.2010) promoted her to consult the local gynaecologist who recognized hematocolpos and let out 100 ml of altered blood by vaginal incision. It temporarily relieved her of pain, however, menstruation did not resume. Hence, she approached out institute on 15.2.11 for further treatment. Clinical examination revealed a firm, nontender, mobile, midline, abdominal mass of 10x6 cm which appeared to be of uterine origin. Tanner stage for secondary sexual characters corresponded to her age. Local examination under anaesthesia revealed normal external genitalia, a hypospadiac urethral meatus, absent vaginal lumen without obvious vaginal bulge due to hematocolpos (cryptomenorrhea).
Ultrasound imaging revealed a 12cm x 4cm mass suggestive of hematocolpos and an unascended right kidney. Intravenous Urography confirmed the unascended right kidney in midline at L3 – L4 level and revealed a duplex collecting system with malrotation on the left side. Both ureters appeared grossly normal and bladder contour revealed extrinsic compression due to pelvic mass. Micturating cystourethrogram revealed a grade IV VUR on the left side. MR urogram recognized the following
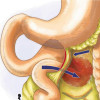
- Posteroinferior bladder diverticulum measuring 37.9mm x 13.8mm with left ureter opening into it (figure i).
- Distal left ureteric diverticulum measuring 14.9mm x 13.6mm (figure i).
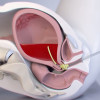
- A bicornuate uterus with hyperintense fluid collection in cervix and vagina confirming the hematocolpos (figure ii).
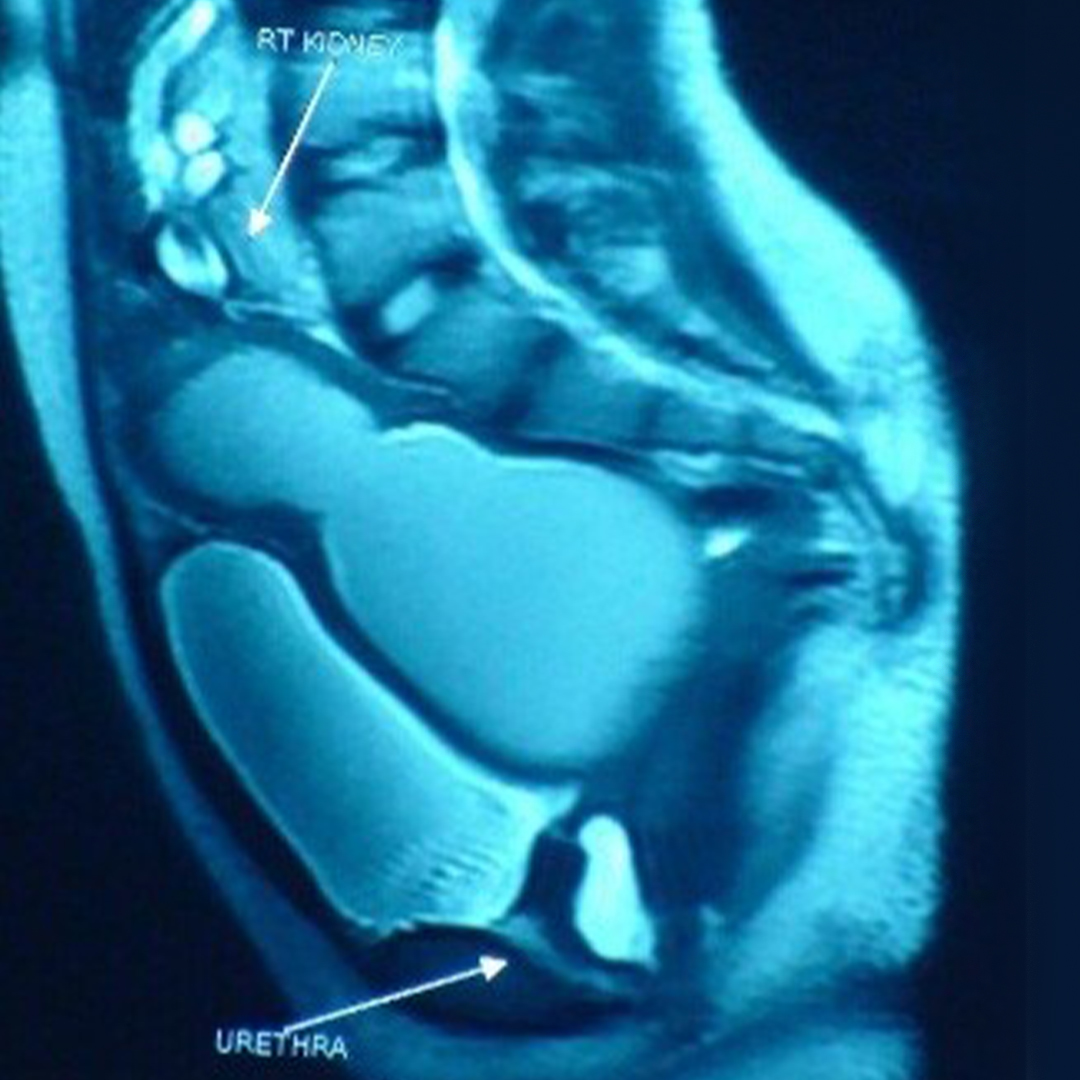

Cystoscopy showed a hypospadiac meatus with short urethra. The trigone was severely distorted and both ureteric orifices were displaced laterally due to the pelvic mass. A wide open left ureteric orifice was entering into the diverticulum of bladder. Further examination revealed an atretic distal vagina and a huge globular mass palpable (rectally) above the atretic vaginal segment.
On 28.3.11 (four months after first attempt) surgical exploration was done. A staged surgical protocol was considered in view of multiple developmental urogenital anomalies.
A “U” shaped incision was made between the perineum and hypospadiac meatus and sharp dissection was required through the hard fibrotic tissue for a distance of 5cm from the fourchette to gain access to the hematocolpos (huge globular mass with thick fibrotic wall). Reaching the hematocolpos through atretic vagina (fibrotic) without injuring the rectum was challenging especially following an unsuccessful past attempt. Per rectal finger guidance facilitated the dissection.
The close proximity of the bladder diverticulum with insertion of left ureter into it forewarned about the possibility of inadvertent injury to bladder or lower ureter during the intervention. To safeguard the left ureter a preoperative retrograde ureteric stenting was attempted which could not be accomplished due to extensive anatomical distortion caused by the mass.
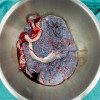
Guidance with foley’s catheter enabled dissection without injuring urinary tract. The hematocolpos was drained by incising its thick fibrotic wall and about 300ml of altered blood was drained.
Post operatively patient was relieved of abdominal pain and resumed her first menstruation 45 days after the surgery. Re-examination during menstruation established the patency of vagina. Post operative micturating cystogram revealed no VUR on left side.
Discussion:
Obstructive lesions leading to hematocolpos require prompt action to relieve pain, retrograde menstruation and pressure effect on adjacent viscera. Restenosis with recurrent mass and pain is a frequent sequel following any vaginal reconstructive surgery which may make future attempts more difficult. During the primary surgical intervention emphasis should be laid on achieving persistent vaginal patency else recurrent hematocolpos and its associated symptoms would demand repeated surgical interventions. Considering the past surgical failure an extensive mobilisation of proximal vagina was carried out which facilitated tension free pull through of proximal vagina through the space created by the lengthy dissection and approximation of its edges to fourchette to form the introitus. Progressive hematocolpos in unobstructed upper vagina resulted in the chronic stretching, distension and elongation of upper vagina and provided adequate length that further enabled the approximation of its edges.
Hematocolpos is a rare cause of external mass compression on the lower urinary tract causing acute urinary retention most likely due to distal vaginal occlusions. However, a long atretic lower vagina even with massive collection only in upper vagina may not feature with urinary retention as it may not compress the outflow tract.
Coexisting bicornuate uterus (mullerian duct anomaly) categories her as class III of the American Fertility Society classification.
The management dilemma in the patient was to combine vesical divertculectomy and ureteric reimplantation of the left ureter (due to significant VUR) in a single sitting during the drainage of the hematocolpos vs. a staged approach. VUR in this case may be congenital or secondary to distortion of the vesicoureteral junction due to bladder diverticula. The vaginal obstruction and hematocolpos is likely to aggravate the distortion and displacement of the lower urinary tract which may be reversible.
VUR could be managed conservatively initially due to the absence of urinary tract infections. Diverticulectomy was not considered as the voiding function was not compromised due to diverticulae. Considering the benefits over risks staged management was adopted. Persistence of reflux or infection will warrant the reimplantation of ureter in future and at the time of reimplantation ureteral and bladder diverticulum will be surgically excised even if it remains asymptomatic.
Usually surgical management of combined multiple developmental anomalies may appear to be complex with prospect of multiple surgical corrections. At times drainage and restoration of continuity and ensuring continued vaginal patency may be adequate to cure the patient. However, patient must be well counseled for sequel like restenosis leading to amenorrhea, pelvic mass and need for further reconstructive surgical interventions.
References:
- Yu TJ, Lin MC (1993) Acute urinary retention in two patients with imperforate hymen. Scand J Urol Nephrol; 27:543-4
- John A. Rock and Lastly L Breech (208) Surgery for anomalies of the mullerian ducts. In: linde’s Operative Gynecology (Tenth edition). Lippincott, Philadelphia, pp 539-84, table 25.2
Author details:
- Prof. N. Rajamaheswari, Professor & Head Department of Urogynaecology, Government Kasturba Gandhi Hospital & Institute of Social Obstetrics, Madras Medical College, Triplicane, Chennai 05, Tamil Nadu, India
- Dr. Sugandha Agarwal, MS (Obstetrics & Gynaecology), Department of Urogynaecology, Government Kasturba Gandhi Hospital & Institute of Social Obstetrics Madras Medical College, Triplicane, Chennai 05, Tamil Nadu, India
- Dr. Archana Bharti Chhikara, Department of Urogynaecology, Government Kasturba Gandhi Hospital & Institute of Social Obstetrics, Madras Medical College, Triplicane, Chennai 05, Tamil Nadu, India
- Dr. K. Seethalakshmi, Assistant Professor, Department of Urogynaecology, Government Kasturba Gandhi Hospital & Institute of Social Obstetrics, Madras Medical College, Triplicane, Chennai 05, Tamil Nadu, India

IJCP Editorial Team
Comprising seasoned professionals and experts from the medical field, the IJCP editorial team is dedicated to delivering timely and accurate content and thriving to provide attention-grabbing information for the readers. What sets them apart are their diverse expertise, spanning academia, research, and clinical practice, and their dedication to upholding the highest standards of quality and integrity. With a wealth of experience and a commitment to excellence, the IJCP editorial team strives to provide valuable perspectives, the latest trends, and in-depth analyses across various medical domains, all in a way that keeps you interested and engaged.
More FAQs by IJCP Editorial Team
slot pulsa
slot pulsa
slot thailand
https://milaanfoundation.org/
slot pulsa
qris
zeus
slot gacor
slot gacor
demo slot
slot88
mahjong
slot gacor
slot gacor
slot gacor
slot88
slot pulsa
slot gacor
akang69
akang69
slot pulsa
akang69
akang69
slot pulsa
slot pulsa
https://chateraise.org/menu/
slot gacor
kanjeng69
https://www.seansprimedining.com/dine
slot gacor
slot demo
akang69
slot gacor
slot pulsa
slot pulsa
akang69
https://valentinesdaycountdown.com/
slot jepang
slot gacor
slot gacor
slot88
slot gacor
slot gacor
akang69
akang69
akang69
akang69
slot gacor
slot gacor
slot gacor
https://www.alpinecafeandbakery.com/menu.html
https://applebeesmenu.us/applebees-lunch-menu/
https://bakeryandsweets-fest.com/product-highlight/
https://sevenseassushi.com/menu/
slot gacor
slot777
https://freakout.club/
slot gacor
slot gacor
https://rsgm.moestopo.ac.id/instalasi-rawat-jalan/
slot gacor
slot pulsa
slot gacor
slot gacor
http://www.motohom.co.in/
slot pulsa
https://intervencion.uahurtado.cl/
slot pulsa
slot pulsa
https://www.kp2.it.maranatha.edu/
slot gacor
slot gacor
mahjong ways
slot gacor
https://azure3.test.utah.edu/
https://iceam.unimap.edu.my/
https://sindika.co.id/contact/
slot gacor
slot gacor
slot pulsa
https://jhep.unimap.edu.my/
slot gacor
Kartu Pokémon Naik Harga!! Penghobi Naik Drastis, Bermain No Limit Dapat Cuan Berlimpah
Resep Putar Hemat WD Paus di Sugar Rush, Murah Namun Ampuh!
Seseorang Terlihat Jauh Lebih Muda dari Usianya, 7 Game Big Bass Crash yang Menguntungkan
Tukang Bubur Demi Beli Honda Megapro Terbaru, Main PGSoft di Kanjeng Jadi Jutawan!
slot gacor
slot pulsa
https://portal.kaafuni.edu.gh/
https://www.thedeenshow.com/
https://elektro.trunojoyo.ac.id/
https://pgsd.trunojoyo.ac.id/
http://www.gmci.in/
https://www.medigunakhisar.com/contact/
https://www.medigunakhisar.com/category/doktorlar/
https://www.medigunakhisar.com/about/
https://www.oscarstores.com/
https://ritalabailaora.com/
https://journal.stiepertiba.ac.id/official/
https://shopifyvps.trackship.co/
https://krandeganbayan.id/
https://www.imik.edu.in/
https://www.natasshaselvaraj.com/
http://ebphtb.banjarnegarakab.go.id/
https://bigbiteonpitt.com.au/
https://sigen.kaltimprov.go.id/
http://rju.parco.gov.ba/
https://samajpragatisahayog.org/
https://bendismea.be.gov.ng/
https://mozaiktravel.id/
https://xm42newdev.wpengine.com/
https://epr.rw/
https://tribelio.page/slotpulsa
https://mhs.akpertgkfakinah.ac.id/
http://lms6.digivarsity.com/
https://ssr.vinayakamission.com/
https://prelnor.molg.go.ug/gallery/
https://englishfocus.upstegal.ac.id/
akang69
https://virtex.canadianminingexpo.com/
slot pulsa
slot bet 200
slot online
convocation.aiou.edu.pk/
https://qna.bpsaceh.com/
https://storage.therapyrooms.com/
https://www.inaexport.id/
https://vmrfdu.edu.in/
https://www.jniemann.it/
https://katalog.intanonline.com/view/
akang69
akang69
akang69
https://affordableadsgroup.com/
https://doktor.fisip.hangtuah.ac.id/
https://um.originmena.com/
https://primemarkets.com.sa/branches
https://primemarkets.com.sa/
https://www.aqtiverse.in/images/
slot gacor
https://rokomarifood.com/
https://beritrust.com/
https://dispora.sumbarprov.go.id/imgs/
slot pulsa
http://pubma.edostate.gov.ng/
https://palermo.if.ua/
akang69
slot qris
http://husc.hueuni.edu.vn/
https://www.grupogasca.com/
slot pulsa
https://ukm.stiedharmaputra-smg.ac.id/
https://ppid.mukomukokab.go.id/
slot gacor
https://s1cs.stmikroyal.ac.id/
https://terlaksana.co.id/img/
slot pulsa
https://graduation.sjctni.edu/SJCGRAD24/abc_id.php
https://admission.sjctni.edu/
https://camarabonitodeminas.mg.gov.br/oficios/
https://kmob.jabarprov.go.id/
https://ssm.school.ssmetrust.in/
https://cjnc.ppnijateng.org/
https://paisaje.age-geografia.es/
slot pulsa
hasilwin
demototo
http://majaslapa.lv/media/
slot gacor
https://sumpah.ppnijateng.org/
https://www.uniabuja.edu.ng/
https://training.super5.org/
slot pulsa
slot gacor
https://mmi.edu.pk/find-a-doctor/
https://lonsuit.unismuhluwuk.ac.id/
slot pulsa
slot gacor
https://taxicarudaipur.com/
slot pulsa
slot gacor
slot gacor
slot gacor
slot pulsa
https://siraberu.mixh.jp/
slot gacor
slot pulsa
slot gacor
https://hkg.methodist.org.hk/
slot gacor
https://www.asopa.org/
https://fisip.unismuhluwuk.ac.id/
slot gacor
https://www.panganku.org/id-ID/semua_nutrisi
https://ejurnal.ikippgribojonegoro.ac.id/
slot gacor
https://katalog.intanonline.com/view/
https://stikesgrahaedukasi.ac.id/
https://kec.slogohimo.wonogirikab.go.id/
https://www.facesulavirtual.net/efaces/
https://www.gratisongkir.id/
https://bukupdpi.klikpdpi.com/
https://ilp.mizoram.gov.in/
https://www.campdoha.org/
slot gacor
slot gacor
https://katalog.intanonline.com/
slot gacor
https://munabarat.go.id/index.php
https://youtube.klikpdpi.com/
https://katalog.intanonline.com/lazada.IM.im-msgbox
https://understandquran.com/
https://youtube.klikpdpi.com/
https://gratisongkir.id/console/
https://gratisongkir.id/vagrant/
https://www.gratisongkir.id/uploads/
https://www.gratisongkir.id/assets/
https://snyderfamilyband.com/
https://handholding.mizoram.gov.in/
https://dconline.mizoram.gov.in/
https://siva.umkendari.ac.id/
https://www.gthlcanada.com/
https://www.gratisongkir.id/assets/
https://www.vidyasthalilawcollege.com/
togel toto
slot gacor
https://www.facesulavirtual.net/
hasilwin
https://amertamedia.co.id/
https://www.gulfstarsauto.com/
https://aptika.id/
https://www.bytestechnolab.com/
slot gacor
slot deposit 10k
slot singapore
slot thailand
AKANG69
AKANG69
https://snyderfamilyband.com/
slot gacor
https://epaper.notunshomoy.com/
https://development.upr.ac.id/
https://fornas.kebijakankesehatanindonesia.net/
slot gacor
slot pulsa
https://e-anatolh.com/
slot gacor
slot thailand
slot pulsa
kanjeng69
https://loudhelp.com/
slot thailand
https://ipss-addis.org/
slot gacor
https://engineering.upstegal.ac.id/
slot gacor
https://sipaksi.unpak.ac.id/
https://pbi.teknik.unmuha.ac.id/
https://bkd.inkhas.ac.id/files/
https://barcode.akbidyahmi.ac.id/
https://sdcirebonislamic.cerdig.com/
https://tilganga.org/
https://siperjaka.ms-langsa.go.id/
slot pulsa
https://dinsos.bekasikab.go.id/
https://stkq.alhikamdepok.ac.id/
http://fmipa.upr.ac.id/
https://beasiswaperintis.id/
slot pulsa
slot pulsa
https://www.thebestflushingtoilet.com/
https://sdiassalaftahfidzulquran.cerdig.com/
https://sv-388.asia/
https://lppm.upr.ac.id/
https://peraturan.upr.ac.id/
https://simpeg-tb.id/
https://contentacademy.id/
https://ws-168.org/
slot pulsa
https://simpeg-tb.id/
https://www.lagrangepointsbrussels.com/
https://admisi.uinsaid.ac.id/img/
slot gatot kaca
https://www.multimarcasgrupovianorte.com.br/
https://silajara.kepulauanselayarkab.go.id/
slot pulsa
https://bapenda.batubarakab.go.id/run/
https://dosen.billfath.ac.id/sites/
gatot kaca slot
http://sibkd.semarangkab.go.id/ekgb/temp/
http://jak.faperta.unand.ac.id/sites/
slot pulsa
slot kamboja
https://dinsos.bekasikab.go.id/yasha/
http://agribisnis.faperta.unand.ac.id/
https://hondayogyakarta.id/
http://jak.faperta.unand.ac.id/sites/
https://dinsos.bekasikab.go.id/hunt/
https://dinsos.bekasikab.go.id/dagger/
http://tanah.faperta.unand.ac.id/potion/
https://dinsos.bekasikab.go.id/dagon/
https://dinsos.bekasikab.go.id/potion/
https://tourism.lgu-santol.gov.ph/
https://fdik.uinmataram.ac.id/rune/
https://v2.poltekpelni.ac.id/fiend/
https://simbada.kalbarprov.go.id/
https://slotpulsa2025.net/
https://slotindosat.net/
https://www.scootersforknee.com/
http://sibkd.semarangkab.go.id/sib/excel/
https://www.worldminner.com/
slot gacor
https://literate.nusaputra.ac.id/lib/
https://potomacofficersclub.com/wp-content/cache/
https://literate.nusaputra.ac.id/docs/
https://literate.nusaputra.ac.id/api/
https://www.idecesar.gov.co/images/
http://sim-epk.poltekkes-medan.ac.id/
http://sibkd.semarangkab.go.id/kartukorpri/pages/
http://sibkd.semarangkab.go.id/kartukorpri/pages/
https://buycapybara.com/
https://desasungaibuluhungar.id/
https://pgmi.unupurwokerto.ac.id/slotzeus/
https://pgmi.unupurwokerto.ac.id/slotthailand/
slot dana
https://admissions.kmtc.ac.ke/
https://permana.upstegal.ac.id/run/
https://permana.upstegal.ac.id/pages/run/
https://stkq2.alhikamdepok.ac.id/
slot pulsa
https://www.allnursejobdescriptions.com/
https://mbkm.uim.ac.id/wp-includes/images/
https://tinjukosimaling.baritotimurkab.go.id/
https://www.silenteye.org/
slot pulsa
https://upscpdf.com/img/
https://keusatker.badilag.net/file_import/
https://bisnis.poltekkesdepkes-sby.ac.id/wp-content/
Slot Bca
Slot Qris
Scatter Hitam
Slot Thailand
Slot Qris
Slot Thailand
Slot gacor
Slot pulsa
Slot zeus
Slot zeus
https://bisnis.poltekkesdepkes-sby.ac.id/wp-content/
https://gresikunited.com/run/
slot gacor
https://pusppm.poltekkesdepkes-sby.ac.id/file/
https://gameplayterbaru.com/
deposit pulsa indosat
https://jdih.tubankab.go.id/js/
https://jdih.tubankab.go.id/library/
https://jdih.tubankab.go.id/img/
https://jdih.tubankab.go.id/gallery/
slot thailand
https://epanel.cblu.ac.in/-/
http://bjkang14.postech.ac.kr/wordpress/
http://bjkang14.postech.ac.kr/wp-includes/assets/
http://bjkang14.postech.ac.kr/wp-includes/images/
https://arktisdesign.com/
https://www.allnursejobdescriptions.com/
https://ziare-online.com/
slot gacor
https://e-jazirah.com/
slot qris
https://www.ultimatepethub.com/
https://slotovo2025.com/
https://www.mobeyday.com/
https://staipati.ac.id/
scatter hitam
slot thailand
scatter hitam
akang69
akang69
akang69
slot qris
slot dana
mahjong ways 3
mahjong wins 3
https://assignmenthacks.com/
Slot Pulsa
Slot pulsa
Slot pulsa
https://acehpos.id/
https://archerysportsindia.com/
https://mrsavnpolytechnic.com/
https://nandanavanamorganics.com/
https://leeupvcsolutions.com/
https://lelaskinclinic.com/
slot thailand
https://thebharatschool.com/
https://mealsandmilemarkers.com/
https://ecustomssecure.com/
https://wallstreetenglish.edu.mm/
https://audio-constructor.com/
https://www.pulsaaxis.net/
https://www.akangseru.com/
https://ukrainemarriageguide.com/
akang69
https://www.akangseru.com/
https://catalinaislandbrewhouse.com/
slot shopeepay
slot shopeepay
10 situs togel
https://captionstore.com/
https://gettranslate.org/
https://terrariumtvultimate.com/
https://www.pryorok.com/
https://saralgyaan.com/
https://ginghameats.com/
slot shopeepay
https://gettranslate.org/
https://captionstore.com
https://enjoyislamabad.com
https://waveites.com
https://voicenusantara.id/
https://mmabreakdown.com/
https://bobmccoyart.com/
https://perpusdajawatengah.id/
https://ziggyoficialbr.com/
slot pulsa
https://linkr.bio/akang69/
https://dev.cfar.org/
https://saveursdailleurs.net/
https://joy.link/akang69
https://ponpesmodernal-imantebelian.ponpes.id/sites/
http://themockingbirdkc.com
http://akang699.kesug.com/
http://akang69.rf.gd/
https://www.ongrace.com/
https://my-home-zen-spa.com/
https://cebofil.org/
http://ironwooddesignstudio.com
https://cebofil.org/
https://pulsa-akang69.tumblr.com/
https://bandar-akang69.tumblr.com/
https://akang69daftar.tumblr.com/
https://sikelor.parigimoutongkab.go.id/vendor/agen-pulsa/
https://www.deviantart.com/slot-gacor-akang69/about
https://www.yuswohady.com/
https://indonesiaindustryoutlook.com/
https://bikeindex.org/users/akang69
https://rivielle.com/
https://issuu.com/akang69
https://heylink.me/akang69z
https://graphicography.id/slotbca/
http://oyannews.com/az/slotdemo/
https://www.laser-travel.com.np/
https://sim-epk.poltekkesjogja.ac.id/slotpulsa/
https://uddoktahoi.com/
http://www.lightcodes.net/
https://wave-gate.lightcodes.net/
https://pohwates-bjn.desa.id/slotdepo/
https://zabava.bluespot.hr/
https://bluespot.hr/
https://www.thethingsnetwork.org/u/akang69/
https://bikeindex.org/users/akang69/
https://www.masterassignment.com/
https://getyourexamdone.com/
https://www.penzion-miromar.cz/
https://sardogs.net/
https://king-lbent.com/
https://lamstyle.com/
https://pulsaindosat.us.com/
https://pulsaindosat.eu.com/
https://pulsaindosat.uk.com/
https://tamilmv.ws/
https://slotindosatt.com/















Please login to comment on this article